Discover subtle warning signs of a heart attack months in advance. Learn what to watch for. Protect your heart health.
A heart attack occurs when there’s a blockage in the blood supply to your heart, typically viewed as a sudden emergency.
Nevertheless, studies reveal that more than 50% of cases involve warning signs up to a month before the event.
Recognizing these symptoms is crucial for seeking prompt medical care.
Harvard Medical School reports that a survey of over 500 female heart attack survivors revealed that 95% noticed warning signs “about a month prior” to the attack.
These red flag symptoms may manifest in the days, weeks, or months, with individual timing variations.

Unusual fatigue ranks as the primary early warning sign, affecting 71% of heart attack survivors surveyed.
It encompasses extreme exhaustion, diminished motivation, and overwhelming tiredness.
Everyday tasks may suddenly feel arduous due to added stress on your heart, which strains to pump blood if there’s a blockage, leaving you drained.
Besides fatigue, other early indicators may involve chest tightness or breathlessness during physical activity. Breathlessness can also result from stress.

Research indicates that more women than men experience these early warning signs. Yet many fail to seek medical attention, assuming these symptoms will subside quickly.

In addition to early warning signs that can manifest days or months before an attack, it’s vital to recognize symptoms during a heart attack. These include:
- chest pressure
- pain radiating to the arms, jaw, neck, back, or abdomen
- dizziness
- sweating
- shortness of breath
- nausea or vomiting
Some individuals may also feel overwhelming anxiety, along with coughing or wheezing. Read more about foods that can help you prevent heart attacks.
Coronary artery disease is the primary cause of most heart attacks, resulting from the blockage of one or more coronary arteries due to cholesterol-laden deposits known as plaques.
These plaques can narrow the arteries, leading to reduced blood flow to the heart. If a plaque ruptures, it can trigger the formation of a blood clot in the heart.
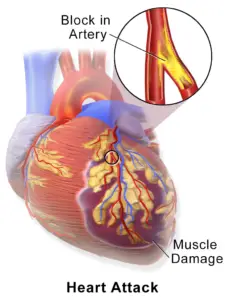
Heart attacks can be categorized based on whether an electrocardiogram (ECG or EKG) reveals specific changes (ST elevation) necessitating urgent invasive treatment.
- An acute complete blockage of a medium or large coronary artery is typically diagnosed as an ST elevation myocardial infarction (STEMI).
- A partial blockage often corresponds to a non-ST elevation myocardial infarction (NSTEMI), although some individuals with NSTEMI may have a total blockage.
It’s important to note that not all heart attacks are caused by blocked arteries. Other factors include:
- Coronary artery spasm, a severe constriction of a non-blocked blood vessel, which can occur in arteries with cholesterol plaques or early vessel hardening due to smoking or other risk factors. This condition may also be referred to as Prinzmetal’s angina, vasospastic angina, or variant angina.
- Certain infections, such as COVID-19 and other viral infections, may lead to heart muscle damage.
- Spontaneous coronary artery dissection (SCAD), a life-threatening condition resulting from a tear within a coronary artery.